Isolated cortical vein thrombosis complicating orbital cellulitis
Abstract
Background: Orbital cellulitis is characterized by the infective inflammation of orbital structures, usually posterior to the orbital septum. Extension of infection from the paranasal sinuses is the most common etiology for orbital cellulitis. Intracranial complications of orbital cellulitis include meningitis, subdural empyema, brain abscess, and cavernous sinus thrombosis.
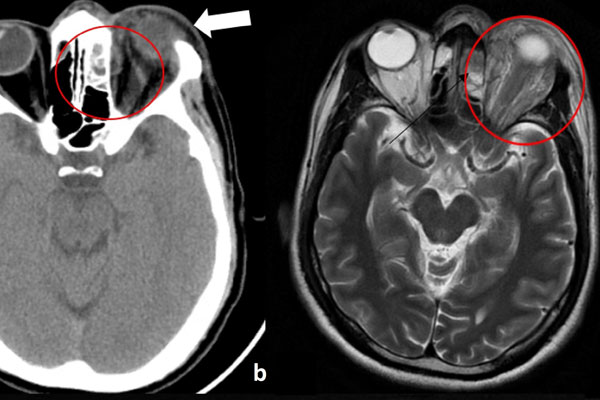
Case presentation: A 33-year-old man presented with acute onset of foul-smelling mucopurulent nasal discharge and swelling of the left eye followed by altered sensorium. On examination of the left eye, chemosis, eyelid edema, and proptosis were present. Computed tomography (CT) of the brain revealed non-axial left proptosis with inflammatory reticulation in the intra- and extraconal fat alongside sinusitis. Magnetic resonance imaging of the brain confirmed the CT findings and additionally showed meningitis and subdural empyema along the left frontoparietal convexity with parenchymal signal changes, suggesting venous infarction in the left frontal lobe. Susceptibility weighted imaging (SWI) confirmed thrombus in the frontal polar vein on the left side, suggesting septic isolated septic cortical venous thrombosis (ICVT) as a complication of orbital cellulitis. Cerebrospinal fluid showed polymorphonuclear cell pleocytosis with elevated protein and lowered sugar. Blood and conjunctival swab cultures were negative. He was subsequently treated with intravenous broad-spectrum antibiotics and antifungals to which he responded and was discharged in stable condition.
Conclusions: Our case highlights the presentation of septic ICVT complicating orbital cellulitis and paranasal sinusitis. It also underscores the higher sensitivity of SWI as a crucial tool in diagnosing ICVT. Appropriate and prompt medical treatment in orbital cellulitis can prevent further complications.
References
Hegde R, Sundar G. Orbital cellulitis: A review. TNOA J Ophthalmic Sci Res. 2017;55(3):211-219.
Chaudhry IA, Al-Rashed W, Arat YO. The hot orbit: orbital cellulitis. Middle East Afr J Ophthalmol. 2012;19(1):34–42.
Chaudhry IA, Shamsi FA, Elzaridi E, et al Outcome of treated orbital cellulitis in a tertiary eye care center in the Middle East. Ophthalmology. 2007;114(2):345-354.
Sepahdari AR, Aakalu VK, Kapur R, et al. MRI of orbital cellulitis and orbital abscess: the role of diffusion-weighted imaging. Am J Roentgenol. 2009;193(3):W244-50.
Singh R, Cope WP, Zhou Z, De Witt ME, Boockvar JA, Tsiouris AJ. Isolated cortical vein thrombosis: case series. J Neurosurg. 2015;123(2):427-433.
Stam J. Thrombosis of the cerebral veins and sinuses. N Engl J Med. 2005;352(17):1791-1798.
Boukobza M, Crassard I, Bousser MG, Chabriat H. MR imaging features of isolated cortical vein thrombosis: diagnosis and follow-up. Am J Neuroradiol. 2009;30(2):344-348.
Chandler JR, Langenbrunner DJ, Stevens ER. The pathogenesis of orbital complications in acute sinusitis. The Laryngoscope. 1970;80(9):1414-1428.
Aribandi M, McCoy VA, Bazan III C. Imaging features of invasive and noninvasive fungal sinusitis: a review. Radiographics. 2007;27(5):1283-1296.
Chang YS, Chen PL, Hung JH, et al. Orbital complications of paranasal sinusitis in Taiwan, 1988 through 2015: Acute ophthalmological manifestations, diagnosis, and management. PloS One. 2017;12(10):e0184477.
Schupper AJ, Jiang W, Coulter MJ, Brigger M, Nation J. Intracranial complications of pediatric sinusitis: identifying risk factors associated with prolonged clinical course. Int J Pediatr Otorhinolaryngol. 2018;112:10–15.
Khatri IA, Wasay M. Septic cerebral venous sinus thrombosis. J Neurol Sci. 2016;362:221–227.
Chatterjee D, Radotra BD, Vasishta RK, Sharma K. Vascular complications of tuberculous meningitis: An autopsy study. Neurol India. 2015;63(6): 926–932.
Konar S, Gohil D, Shukla D, et al, Arimappamagan A, Devi BI. Predictors of outcome of subdural empyema in children. Neurosurg Focus. 2019;47(2):E17.
Kojan S, Al-Jumah M. Infection related cerebral venous thrombosis. J Pak Med Assoc. 2006;56(11):494–497.
Copyright (c) 2020 Vivek S. Murumkar, Karthik Kulanthaivelu, Sheetal Goyal, Shamick Biswas

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors who publish with this journal agree to the following terms:
- Authors retain copyright and grant the journal right of first publication, with the work twelve (12) months after publication simultaneously licensed under a Creative Commons Attribution License that allows others to share the work with an acknowledgement of the work's authorship and initial publication in this journal.
- Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the journal's published version of the work (e.g., post it to an institutional repository or publish it in a book), with an acknowledgement of its initial publication in this journal.
- Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their website) prior to and during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See The Effect of Open Access).


